
Post 44: Before You Say Yes to Scoliosis Surgery: What 25 Years in Clinics Taught Me to Try First
The surgeon shows you the x-ray. The curve is worse than last year. He points to the numbers — 45 degrees, 60 degrees — and tells you that if you wait much longer, the window for the best surgical outcome will close.
You nod. You take the pamphlet. You schedule the follow-up. And somewhere on the drive home, a quiet question forms that you're almost afraid to say out loud:
Is surgery really the only option?
I want to talk to you about that question. Not to dismiss your surgeon, not to tell you what to do, and not to pretend this is simple. But because after more than 25 years as a pediatric physiotherapist, manual osteopath and fascia therapy specialist — including five years working inside an orthopedic hospital gait lab, sitting beside surgeons as they planned these exact procedures — I have seen enough of the long game to believe you deserve a fuller picture.
What I Learned in the Gait Lab
When I worked in the orthopedic hospital, my job was to analyze how children moved. I would spend three hours with a child — cameras, sensors, detailed observation — and then sit with the surgical team to interpret the data and plan their intervention. I was in the room when the decisions were made. And then, because I was also doing the post-surgical rehabilitation, I was there for what came after.
Many of those outcomes were genuinely good. I want to be honest about that. Surgery, when it is truly needed, can change a child's life.
But I also watched what the textbooks don't document. I saw children who lost head control they had worked years to build — after a procedure that was supposed to help them. I saw teenagers in pain from hip surgeries that looked beautiful on x-rays but left them unable to stand. I saw adults I'm still in contact with today, decades later, who tell me their feet look straighter but they can't bear weight because the pain never went away.
And I watched as the surgeons, year after year, presented their outcomes at congresses — counting x-rays, not children. Showing before-and-after images of spines, not before-and-after stories of families. Nobody was asking: what is this child's quality of life now? Is she in pain? Can she breathe more easily? Does she sleep?
Function is always more important than shape. A spine that looks better on an x-ray but leaves a child in more pain is not a better spine.
The Problem With How Scoliosis Is Measured
Here is something I want every parent to know before they sit in that appointment again.
Most scoliosis measurements in children with cerebral palsy are taken on x-rays captured while the child is sitting. And children with CP — especially those with low trunk tone, abdominal weakness, or fascial tension patterns — collapse in sitting. That collapse is real, and it contributes directly to how curved the spine looks in that image.
When you measure the curve of a collapsing spine, you are not measuring the spine. You are measuring the collapse.
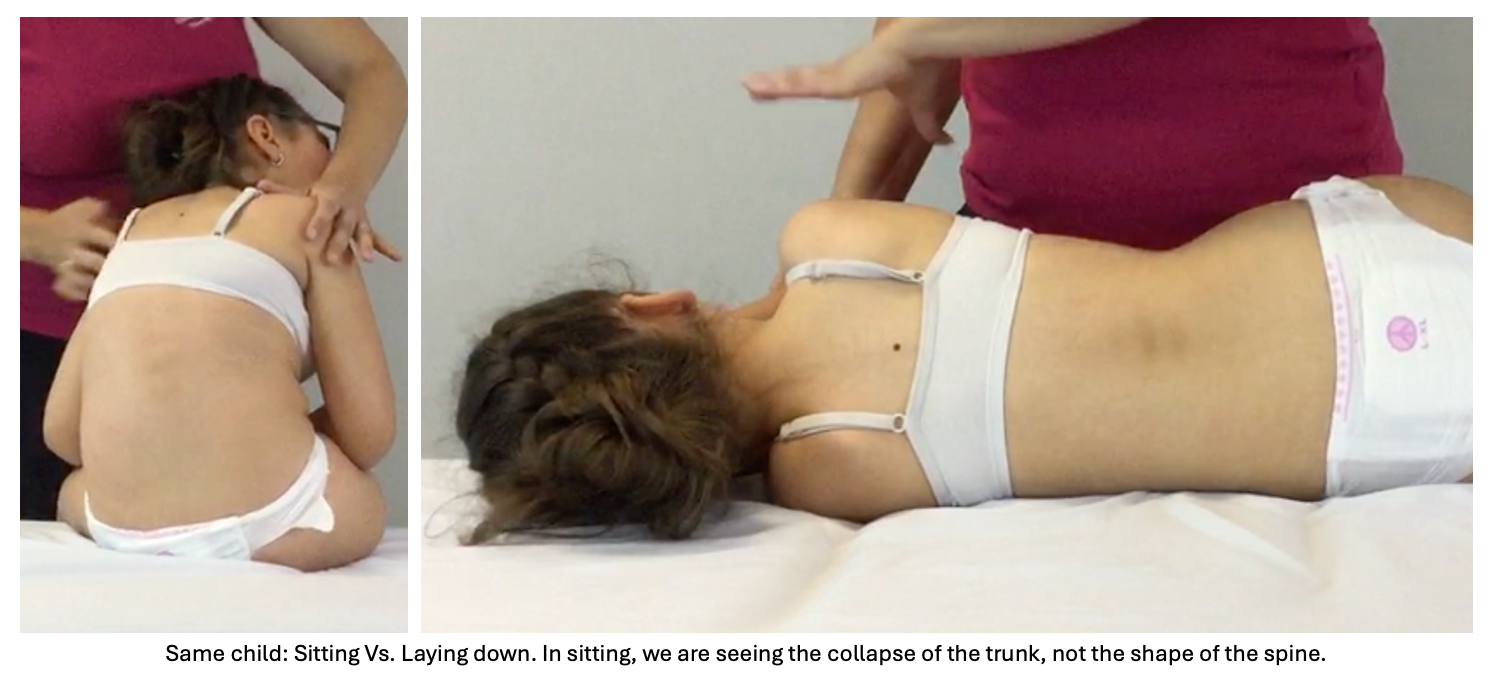
I ask the families I work with to find out one thing: were the x-rays taken in sitting, or lying down? In lying, gravity is no longer pulling the child into collapse. The spine is free to show you what it can actually do. A curve that looks severe in sitting will often look meaningfully different in lying — and that difference is clinically important.
So before any surgical decision is finalized, I would encourage you to ask your surgeon directly:
"Were these measurements taken in lying? Can we compare a lying-down x-ray alongside the sitting one?"
You are not being difficult. You are being a good advocate. And some surgeons will welcome it — because the good ones already know this matters.
The Spine Is Not a Tower of Bones
The mechanical model of scoliosis goes something like this: the spine is misaligned, so we align it. We use hardware, rods, fusions — we impose the shape we want and hold it there.
This model has its place. But it leaves out something fundamental about how a living body actually works.
Every vertebra in your spine is floating in fascia. Not fused to the one above or below it — floating, suspended in a continuous web of connective tissue that runs from the crown of your head to the soles of your feet. What keeps the spine aligned is not the bones themselves. It is the tensional balance of the entire system around those bones.
If this idea is new to you, Fascia's Role in Posture, Head Control, and Torso Stability is a good place to start — it explains how the connective web holds the whole body together, and why working with it changes things that stretching and strengthening alone cannot.
Think of a tent. If the internal poles are weak and the guy ropes are uneven, the tent sags and twists. You could come in with clamps and force it into a better shape — but the moment you remove the clamps, it sags again. Or, you could work on the ropes. You could rebalance the tension. You could strengthen what holds the structure from within. And then the shape corrects itself — not because you forced it, but because the system found its own balance.
That is what fascia therapy is doing. Not forcing. Not correcting. Helping the system find better balance so the shape can change from the inside.
If you want to go deeper into how scoliosis and fascia are connected in children with CP, I wrote a full post on this — The Spine and Scoliosis in Children with Cerebral Palsy — which walks through the science with real case examples.
Why Scoliosis in CP Is Often a Breathing Problem
This is the part of the conversation that almost never happens in the orthopedic office, and I believe it is the most important part.
What keeps the spine flexible — what keeps every single vertebra moving the way it should — is not the therapy you do twice a week. It is breathing. Twenty-four hours a day, every time the diaphragm descends and the ribcage expands, each rib moves. And that movement, sustained around the clock, is what keeps the thoracic spine supple, mobile, and adaptable.
In a child with cerebral palsy who has significant trunk tone changes, the ribcage is often compressed. The diaphragm is not descending fully. The ribs are barely moving. And so the 24-hour natural mobilization of the thoracic spine — the thing that keeps it from stiffening — is simply not happening.
I wrote an entire post about why breathing deserves far more attention than it gets — Breathing and Cerebral Palsy: Why It Matters More Than You Think — because this connection is one of the most overlooked pieces of the scoliosis puzzle.
Of course the spine tightens. Of course the curve progresses. The mechanism that was designed to maintain it has been switched off.
When we work on the chest and the abdomen in fascia therapy — when we release the fascial tension that is holding the ribcage compressed — we are not treating the scoliosis directly. We are restoring the conditions that allow the spine to maintain and reorganize itself. We are switching the mechanism back on.
What I Have Seen Is Possible
I want to show you, not just tell you.
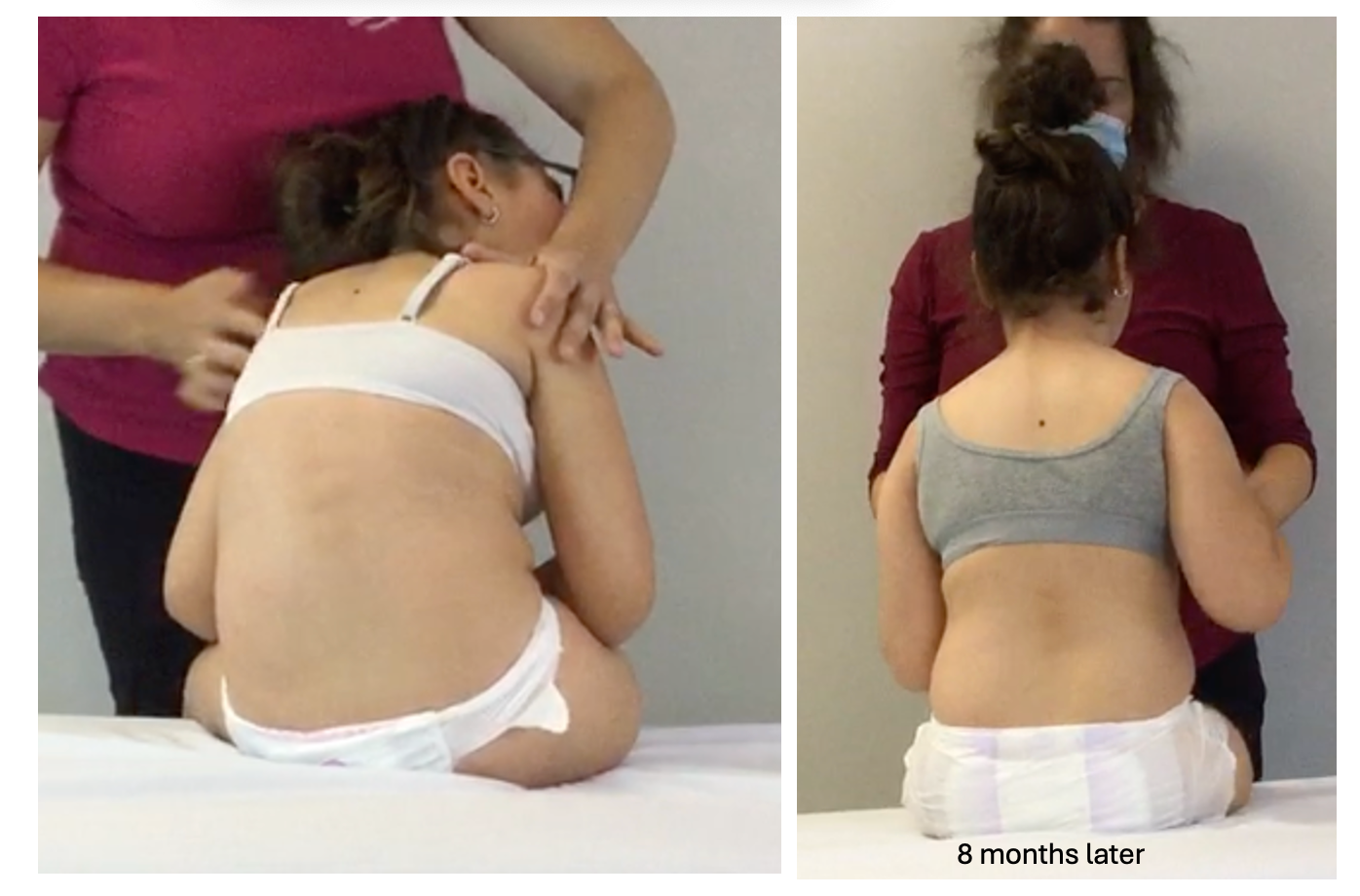
A girl came to my office at age nine with a clear rotational scoliosis. Her parents had been told surgery was being considered. I asked them to wait, and we started working together. Over the following year — by implementing a consistent home routine her parents carried out — her posture changed. Her spinal flexibility increased. Her collapse in sitting reduced. The surgery was never needed. She is 15 now, doing well, and her family has not been back to the orthopedic surgeon in years. Not because they are avoiding it, but because there has been nothing to go back for.
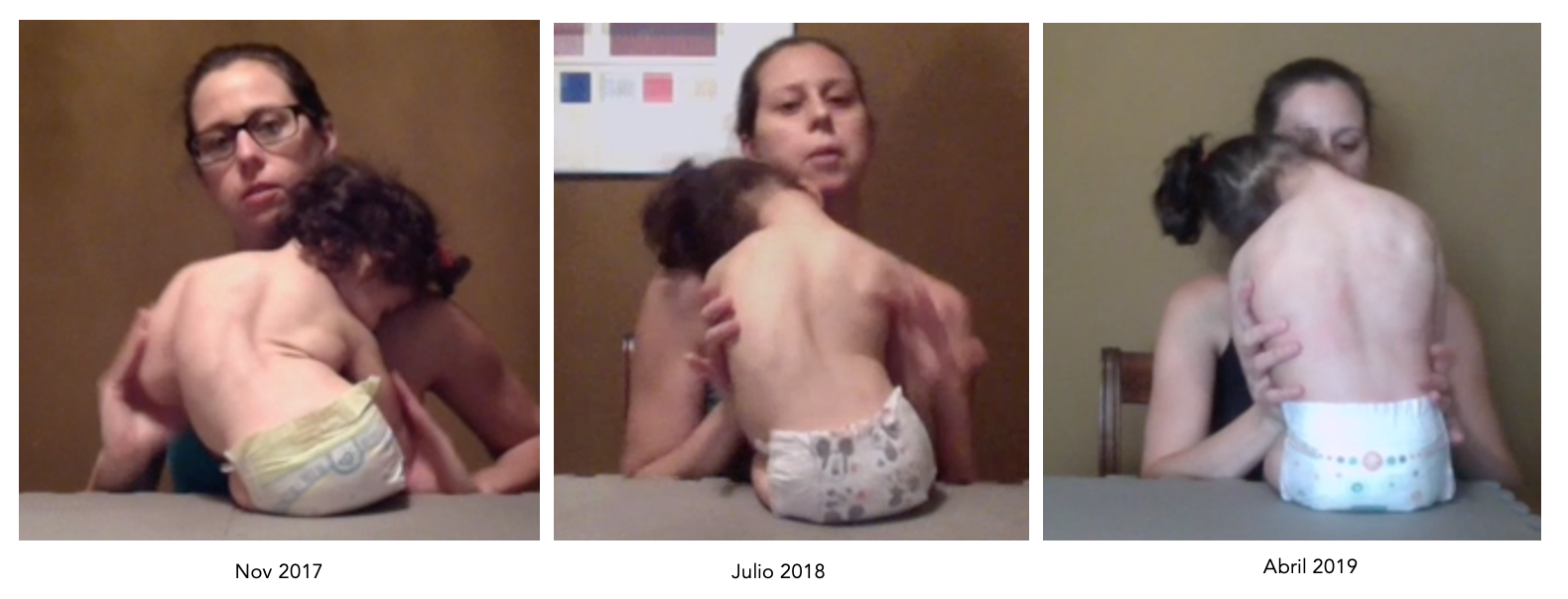
Another family — working remotely, in Venezuela, a severely involved child I have never seen in person — sent me photos every few months. The change in her trunk organization over 18 months was unmistakable. Not perfect. But real, meaningful, and moving in the right direction.
It is never too late. The only time it is truly too late is when the structure has been surgically fused — because we cannot undo that.
What to Ask Before Any Surgical Decision Is Made
If you are in the process of evaluating scoliosis surgery for your child, here are the questions I would bring to every appointment. Write them down. Ask them out loud. You are not overstepping — you are doing exactly what a good parent should do.
1. Were the x-rays taken in sitting or lying down?
Ask to see measurements from both positions if possible. The difference is often significant. If measurements have only been taken in sitting, request a lying-down x-ray before any final decision.
2. How flexible is the curve?
A flexible curve — one that partially corrects when your child is lifted or supported — is very different from a rigid one. Flexibility suggests the system still has room to respond. Ask your surgeon to test this. Ask them to show you what the spine does when gravity is removed.
3. What is the long-term quality-of-life data for children at my child's level of involvement?
Not x-ray outcomes. Not radiographic measurements. Quality of life: pain, respiratory function, ease of care, sleep, comfort. Ask for that data specifically.
4. What happens if we wait six months and do intensive conservative therapy first?
In most cases, six months of focused fascia work will not close a surgical window permanently. Ask your surgeon directly whether a structured trial of conservative therapy — with clear reassessment markers — is a reasonable option before committing to surgery.
5. What are the known risks and long-term complications at this level of surgery?
Not the brochure version. The honest, complete version. How many children at this GMFCS level have had complications? What is the rate of adjacent-segment changes after spinal fusion? Are there families you can speak with who are five or ten years post-surgery?
None of these questions are adversarial. They are the questions of a parent who is taking the decision seriously — and any surgeon who is genuinely working in your child's interest will respect them.
What I Am Not Saying
I want to be clear, because I think this matters.
I am not saying surgery is never the right answer. There are children for whom it is genuinely necessary — where respiratory function is at risk, where the curve is severe and rigid, where conservative options have been exhausted. I have worked with those families too, and I respect those decisions.
I am also not asking you to carry guilt about choices you have already made. Whatever surgery your child has already had — whatever path you took with the information and support you had at the time — was done out of love. That is enough. We work with where we are, always.
What I am saying is this: the body is not a machine. The spine is not a tower of independent parts. And the question — is surgery really the only option? — deserves a full, honest answer before you walk into that operating room.
And if there is one shift I would invite you to make as you sit with that question, it is this: stop trying to fix your child, and start trusting them. That post is one of the most important things I have written, and it is the foundation everything else here rests on.
You deserve that answer. Your child deserves that answer.
In 25 years, I have never damaged a child with fascia therapy. The worst outcome is that it doesn't work as fast as we hoped. That is a very different risk than the one on the surgical consent form.
Ready to Start?
Take your first step into fascia therapy with our short, parent-friendly workshop:
The #1 Fascia Therapy To Improve Torso Control
Gentle, effective, and easy to begin—no experience needed.
Want to Go Deeper?
If you’re ready to fully embrace this gentle approach and receive personalized support, apply for TheraParent Coaching—our therapeutic coaching program designed for dedicated parents like you.
Includes weekly calls, a tailored plan, and a supportive community.
Apply here – it’s free to explore.
Stay connected and inspired every week.
Subscribe to our weekly blog updates and receive new posts, encouragement, and fascia therapy tips right in
your inbox. So never miss the support and ideas that can make a difference in your journey.
